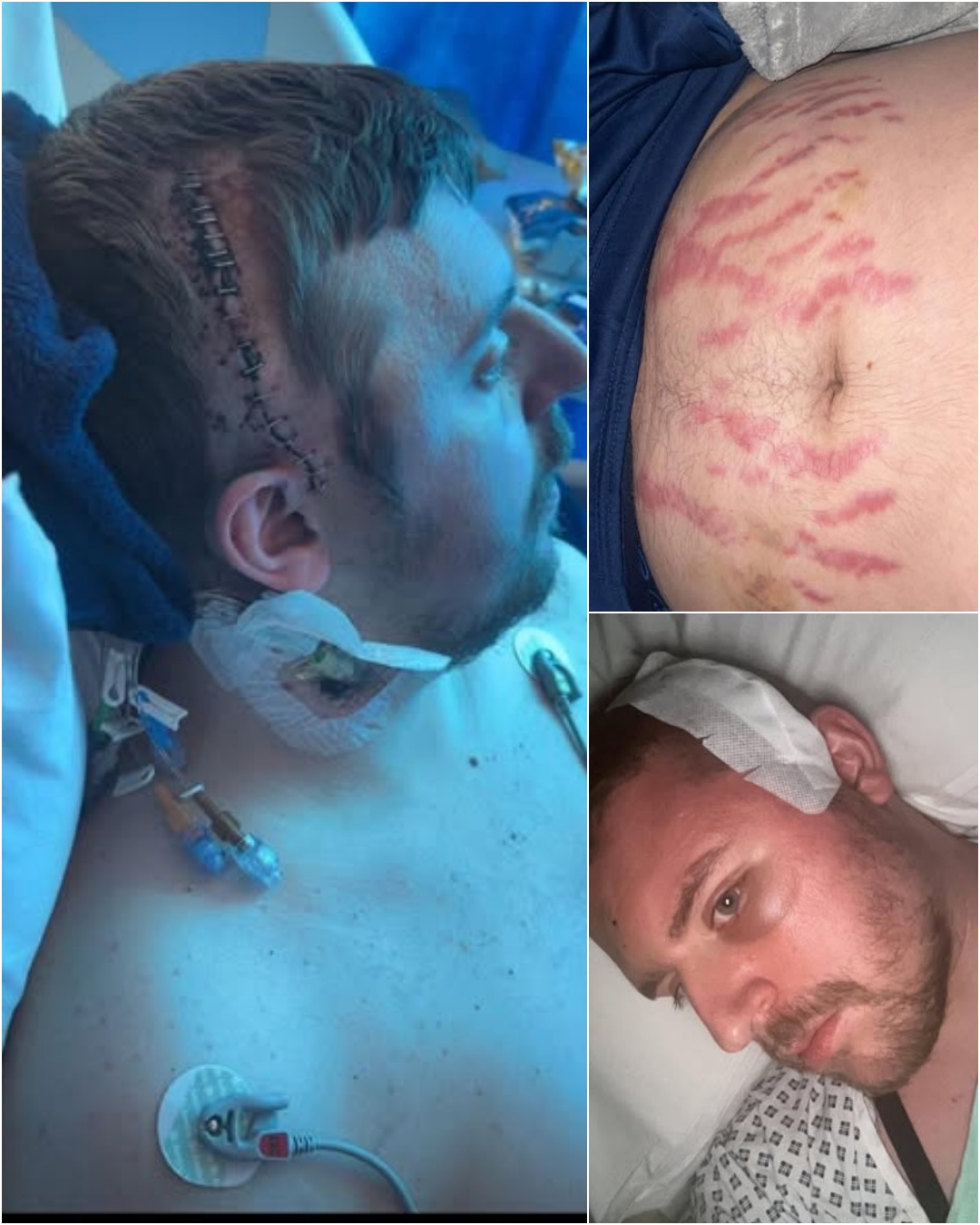
Jason Taylor was 32 years old and in peak health when his life split cleanly into before and after. He exercised. He worked. He made plans like anyone else his age, assuming time was something steady and predictable. Then the seizures started.
At first, they felt unreal — sudden, violent interruptions in a body that had never betrayed him before. One moment he was standing. The next, he was waking up confused, surrounded by worried faces. Scans were ordered. Specialists were called. And then came the words that hollow out a room.
A massive brain tumor.
Six to seven centimeters.
It was not small. It was not incidental. It was large, aggressive in presence, pressing against areas of his brain that controlled movement, speech, and survival itself. Jason went from routine appointments to surgical consults in what felt like hours. He remembers fragments — the antiseptic smell of hospital corridors, the seriousness in doctors’ eyes, the weight of understanding that this was not minor.
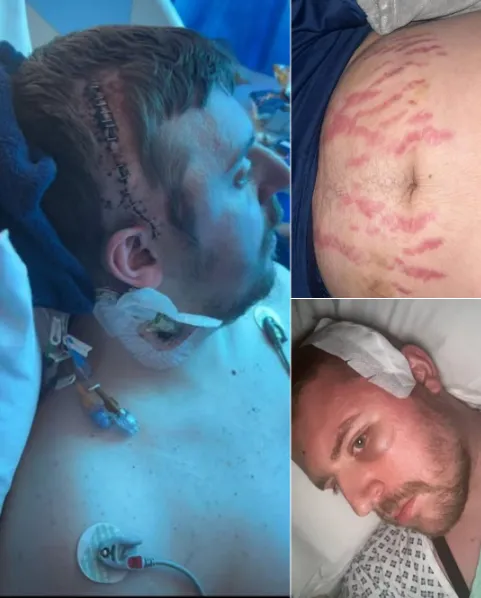
Brain surgery was scheduled.
There are few phrases more terrifying than “we need to operate on your brain.” It is where identity lives. Memory. Personality. The very essence of who someone is. Jason signed consent forms knowing the risks included paralysis, bleeding, cognitive changes — even death.
The surgery was long. Complex. Delicate.
When he woke up, nothing was simple.
Complications stacked one on top of another. An induced coma. Paralysis. Deep vein thrombosis. Brain bleeds. Days blurred into nights filled with alarms and urgent voices. Twice, doctors warned his family he might not survive. Twice, conversations happened in hallways about preparing for the worst.
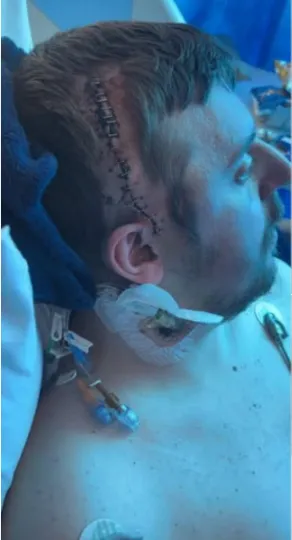
Jason doesn’t remember all of it. Some of those days exist only in stories told back to him later. But he remembers enough — flashes of fear, the crushing weight of weakness, the realization that his body no longer responded the way it once had.
Paralysis steals more than movement. It steals independence. The ability to stand when you choose. To walk out of a room. To reach without thinking. For a man who had once been strong and active, it was disorienting and devastating.
And yet, he survived.
The tumor was removed. The pathology reports came back. The scans eventually showed what once seemed impossible: tumor-free.
But survival did not mean the fight ended.
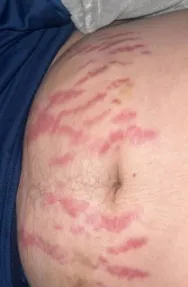
Recovery from brain surgery is not a straight road. It is jagged. Unpredictable. Filled with setbacks that feel unfair. Jason battled not only physical weakness but blood clots, internal bleeding, and relentless pain that made even rest exhausting. Rehabilitation became his new full-time occupation. Every movement had to be relearned. Every step reclaimed.
There is a visible side to trauma — scars along his scalp, the memory of tubes and IV lines. And then there is the invisible side.
PTSD.
Anxiety.
Depression.
These do not show up on MRI scans. They do not fade with stitches removed. They linger quietly in the background — in sudden flashes of panic, in sleepless nights replaying near-death warnings, in the heavy awareness that life can change without permission.
May you like
Jason asks himself often, “How am I still alive?”

It is not asked in disbelief alone. It is asked with gratitude, confusion, and sometimes guilt. When doctors prepare families for goodbye and the goodbye doesn’t come, it leaves a complicated imprint. Survival can feel both miraculous and overwhelming.
Through it all, Jason credits his “fellow warriors.”
Friends who sat in hospital chairs longer than comfort allowed. Family who refused to let hope dim even when medical updates were grim. Supporters who sent messages, prayers, encouragement — reminders that he was not fighting alone.
Community became oxygen.
There were days when giving up would have been easier. Days when progress felt microscopic. But someone was always there — reminding him of the miles already traveled. Reminding him that paralysis did not erase strength. That fear did not erase courage.
Today, Jason is tumor-free.
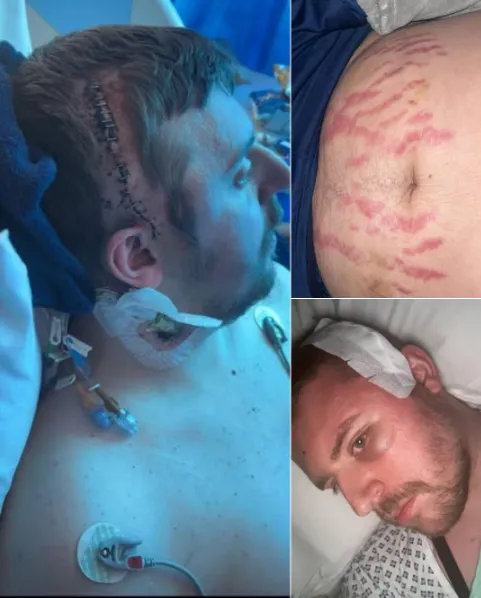
That sentence carries enormous weight. It carries gratitude. It carries relief. But it does not erase the ongoing battle. Healing is layered. Physical therapy continues. Mental health support matters. Recovery is measured not just in scans, but in mindset.
He is rebuilding.
Piece by piece.
The man who once moved without thinking now celebrates simple milestones. Standing. Walking. Breathing deeply without pain. Laughing without fear of the next seizure. These are no longer assumed — they are treasured.
Jason’s story is not one of instant triumph. It is one of relentless endurance. Of surviving the operating room. Surviving the coma. Surviving the warnings. And then choosing, daily, to survive the aftermath.
He still asks, “How am I still alive?”
Maybe the better question is this:
What will he do with the life he fought so hard to keep?
For now, he keeps showing up. For therapy. For conversations. For the people who never left his side. He keeps fighting the invisible battles as fiercely as he fought the tumor.
And if there is one thing his journey makes clear, it is this:
The tumor is gone.
The warrior remains.
Holding On in the ICU: DJ Daniel’s Fight Through a Fragile Night 6508
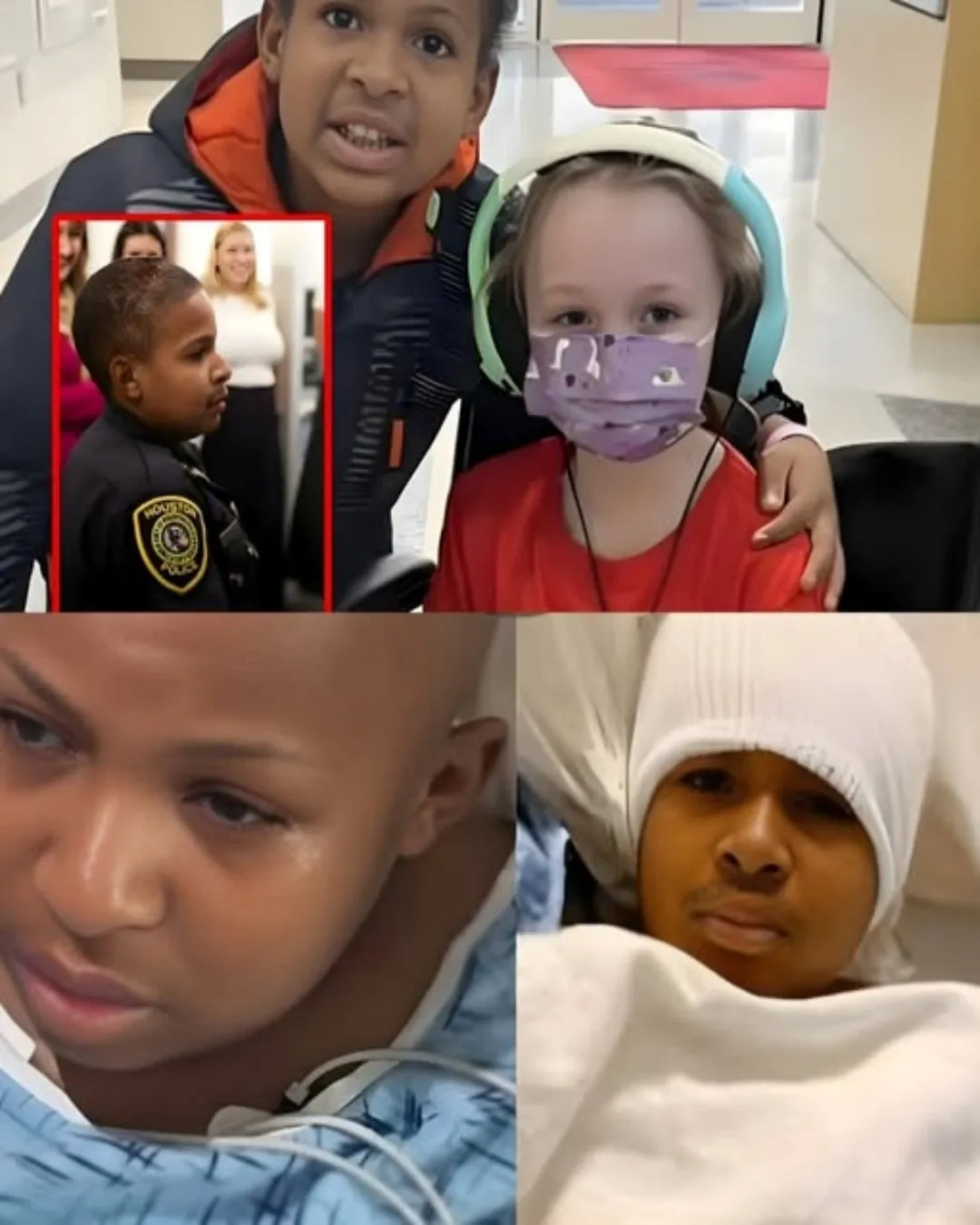
There are moments in a medical journey when everything feels balanced — carefully managed, cautiously hopeful — and then there are moments when that balance shifts without warning. For DJ Daniel, that shift came quickly. What began as concern over rising symptoms escalated into a medical emergency marked by a rapidly climbing fever and critically low blood counts. Within hours, what had been routine monitoring turned into urgent intervention.
His medical team acted immediately.
There was no hesitation.
When lab results signaled danger and his temperature spiked beyond safe limits, doctors and nurses moved with practiced urgency. Medications were administered. Fluids were adjusted. Emergency protocols were activated to stabilize his body before the situation could spiral further. In cases like DJ’s, minutes matter. The difference between stability and crisis can be measured in numbers flashing across a monitor.
He was transferred into intensive care.
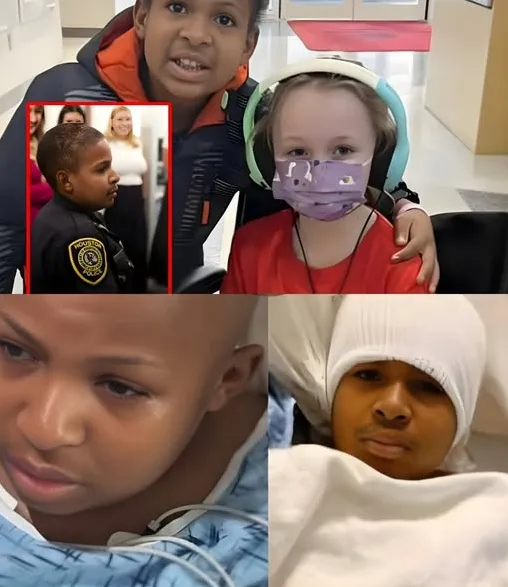
Inside the ICU, everything changes. The lights never fully dim. Machines hum in steady rhythm. Monitors display heart rate, oxygen saturation, blood pressure, and neurological responses in real time. Every sound carries meaning. Every change is noticed.
DJ now remains under constant, minute-by-minute observation.
ICU specialists are tracking his vital signs closely. His lab values are being reassessed repeatedly to watch for any further drops in blood counts or signs of infection. Neurological responses are evaluated carefully, ensuring that his body is not only surviving but functioning as it should. In complex medical situations like his, stability can be delicate. What looks steady one hour can shift the next. That is why the current focus is unwavering: maintain balance, prevent complications, respond instantly to any change.
Recent imaging and diagnostic scans are under detailed review.
Radiologists and specialists across multiple disciplines are examining every detail. Oncology, critical care, infectious disease consultants, and other teams are coordinating in real time. Adjustments are being made based on how DJ’s body responds — tweaking medications, recalibrating supportive therapies, reassessing next steps hour by hour rather than day by day.
There is no single doctor carrying this alone.
This is coordinated medicine.
Layered expertise.
Care that moves like a network rather than a straight line.
In situations involving compromised immune systems and unstable blood counts, the risk of infection increases dramatically. A rapidly escalating fever is not just uncomfortable — it is dangerous. It signals that the body is fighting something it may not be fully equipped to handle. That is why aggressive treatment began immediately: antibiotics, supportive therapies, protective protocols designed to shield him from further exposure.
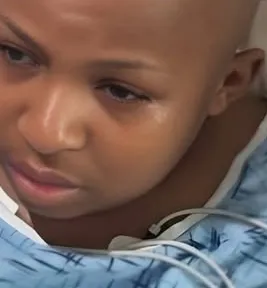
But medical care, as advanced as it is, is only one part of the story.
Outside the hum of machines and the glow of monitors, his family sits close.
They are watching numbers.
Watching his chest rise and fall.
Watching doctors move with steady hands.
They are leaning on faith in a room that tests it.
When someone you love is in intensive care, time behaves differently. Minutes stretch. Updates feel monumental. A small improvement becomes cause for quiet celebration. A stable reading feels like relief you didn’t realize you were holding your breath for.
His family has asked for continued prayers.
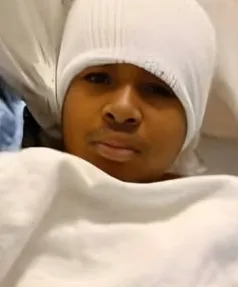
For privacy.
For compassion.
They understand that intensive care is not measured in dramatic breakthroughs. It is measured in guarded stability. In hours without decline. In lab values that stop falling. In fevers that slowly, carefully begin to respond to treatment.
Right now, the priority is clear.
Stabilization.
Protection.
Continuous oversight.
There are no promises in critical care. Only effort. Only vigilance. Only teams of professionals adjusting and readjusting based on what his body communicates. The road ahead may be uncertain, but it is not unattended. Every available resource is being directed toward supporting his recovery.
Progress in the ICU rarely looks dramatic.
It looks like numbers that hold steady.
It looks like small improvements guarded carefully.
It looks like doctors saying, “He’s stable,” and knowing that stability is victory for now.
DJ Daniel is not alone in this fight.
He is surrounded by specialists.
By technology.
By family who refuse to leave his side.
And by a community hoping for the moment when crisis turns into recovery.
For now, the focus remains steady.
Keep him stable.
Keep him protected.
Keep moving forward — one carefully monitored step at a time.